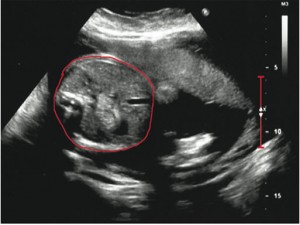 
The fetal heart rate should be between 110 and 160 beats per minute during the third trimester of pregnancy and labor. It is most commonly measured via electronic fetal monitor. Doctors can use internal or external tools to measure the fetal heart rate (1). The fetal heart rate should be monitored throughout pregnancy and taken at every prenatal appointment. Post-term pregnancy (pregnancy at 42 weeks or more)įetal distress is diagnosed based on fetal heart rate monitoring.Causes of fetal distress Some common causes of fetal distress include (1): Instead, the term “nonreassuring fetal status” has been more commonly used to describe the clinician or doctor’s interpretation of the data related to fetal status. 
In fetal distress, the baby appears to be lacking adequate oxygen based on fetal heart rate, though the cause may not be known. Birth asphyxia means that the baby is not receiving adequate oxygen during labor or delivery because of an issue like cord compression, placental abruption, or another birth complication. However, many doctors still use the phrase. Īccording to an American College of Obstetricians and Gynecologists (ACOG) Committee Opinion in 2005, the term fetal distress was deemed too confusing, as it was very similar to “birth asphyxia” (2). If fetal distress goes unmanaged it can lead to more severe injuries such as hypoxic-ischemic encephalopathy (HIE). When a baby is in distress they may require immediate intervention, such as delivery by C-section or certain methods of intrauterine resuscitation. Fetal distress is an indication that the baby may not be doing well in utero. What is fetal distress?įetal distress, also called “nonreassuring fetal status,” is the term medical professionals use to describe when a fetus is not receiving adequate oxygen during pregnancy or labor (1). Please call 911, your country’s emergency number, or your doctor if you may be having a medical emergency. (2014, October 16).Disclaimer: We cannot provide treatments or medical advice. Ruptureof membranes: has your water broken Low amniotic fluid levels: oligohydramnios.(2015, August).Amniotic fluid: physiology and assessment.You can learn more about how we ensure our content is accurate and current by reading our editorial policy. Healthline has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. If you do this and don’t see any fluid on the pad, the fluid you are seeing is probably urine. If it isn’t, the fluid could be amniotic fluid.Īnother option is to put on a pad or panty liner and concentrate on holding your pelvic floor muscles tight, as if you are trying to stop your urine stream. If the fluid is yellow in color, it’s likely urine. Place a sanitary pad or panty liner in your underwear and examine the fluid that is on the pad after 30 minutes to an hour. Vaginal fluid is usually white or yellow in color.Īnother way you can try to determine if the fluid is amniotic fluid is to first empty your bladder. clear, white-flecked, and/or tinged with mucus or blood.So it can be difficult to determine if fluid is urine, amniotic fluid, or vaginal fluid.Īmniotic fluid may have a few of the following qualities: Your vaginal tissues also may produce extra fluid to help your baby pass more easily. When you’re pregnant, you may feel like everything leaks: Your bladder becomes fuller faster, and you may leak urine. This can result in a slow leak of amniotic fluid. While it’s possible to break the water balloon, causing a strong gush of fluid (known as your water breaking), it’s also possible that a small hole could develop in the sac. Think of your amniotic sac like a water balloon.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
